Full benefits of electronic health records only accrue with the implementation of effective retrieval and reuse of clinical information. The scope of analysis of health record data may cover:
- An individual patient, across time and/or care providers;
- An individual healthcare worker;
- Patient groups or cohorts, based on demographics, diagnoses, treatments or interventions;
- Enterprise groups, based on teams, wards, clinics, institutions or providers;
- Geographical groups, based on a local area, town, region or country.
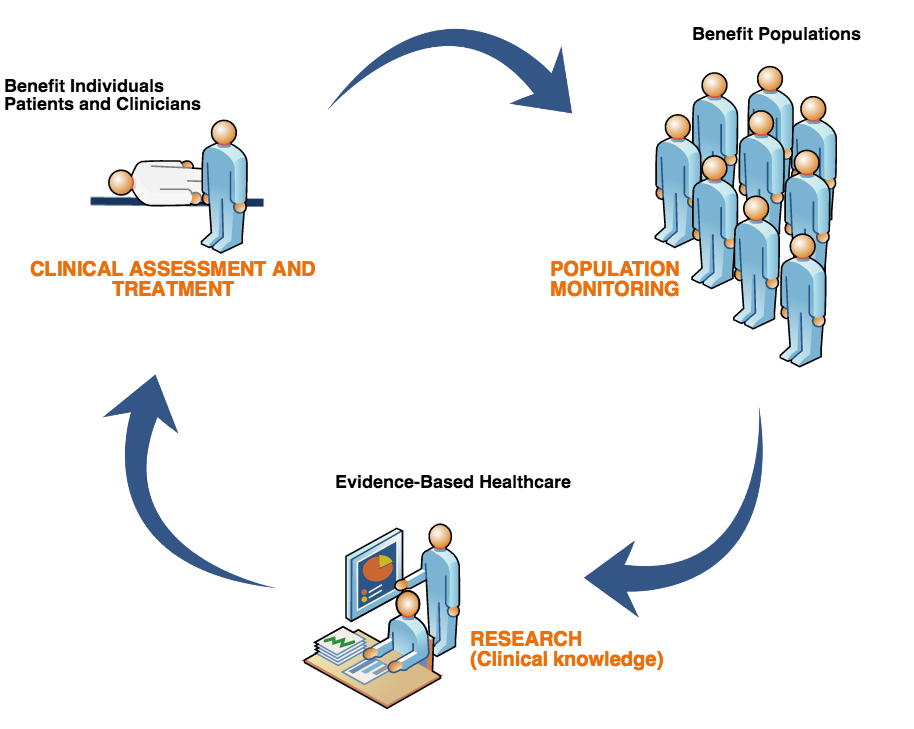
Figure 3.2-1 illustrates the three main purposes of analytics with SNOMED CT. These are:
- Clinical assessment and treatment;
- Population monitoring; and
- Research.
Figure 3.2-1: Purposes of analytics with SNOMED CT
SNOMED CT may be used to support analytics that:- Improves the care of individual patients by enabling:
- Retrieval of relevant information that better supports clinicians in assessing the condition and needs of a patient
- Clinical records to be integrated with decision support tools to guide safe, appropriate and effective patient care – for example, allergy checking and potential drug contraindications identified at the point of prescribing
- Reduction in the duplication of investigations and interventions through the effective retrieval of shared information about the patient
- Meaning-based sharing of clinical information that is collected by different members of the health care team at different times and places (and potentially in different languages)
- Identification of patients requiring follow-up or changes to treatment based on updated guidelines
- Wellness management, for example, using genetic and behavioral risk profiles.
- Context-sensitive presentation of guidelines and care pathways within the user interface
- Labor-saving decision support systems for clinicians
- Adaptive pick lists in clinical user interfaces
- Professional logs and performance tracking for clinicians
- Work list generation, for example, patients requiring follow-up based on specific criteria
- Workload profiling and monitoring.
- Improves the care of populations by enabling:
- Epidemiological monitoring and reporting, for example, monitoring of epidemic outbreaks, or hypothesis generation for the causes of diseases
- Audit of clinical care and service delivery
- Systems that measure and maximize the delivery of cost-effective treatments and minimize the risk of costly errors
- Supports evidence-based healthcare and clinical knowledge research by enabling:
- Identification of clinical trial candidates
- Research into the effectiveness of different approaches to disease management
- Clinical care delivery planning, for example, determining optimum discharge time
- Planning for future service delivery provision based on emerging health trends, perceived priorities and changes in clinical understanding.
Feedback
Overview
Content Tools
Apps